In fertility evaluation, a transvaginal ultrasound is one of the investigations that can quickly provide useful information about the uterus, endometrium and ovaries, especially before In Vitro Fertilization (IVF). It is not merely “a routine ultrasound,” but an assessment that helps clarify the biological context at that moment: what can be seen, what is worth following dynamically and what might require additional checks before starting a protocol.
At the same time, a transvaginal ultrasound can only be interpreted correctly depending on cycle day, medical history and the clinical objective (initial evaluation, monitoring, clarifying symptoms). A high-quality scan performed at the right time can answer important questions without unnecessarily adding investigations.
What a Transvaginal Ultrasound Is and Why It Is So Common in Infertility
A transvaginal ultrasound is an imaging examination performed with a thin probe inserted into the vagina, allowing detailed visualization of the uterus, endometrium, ovaries and the pelvic space. Because the probe is close to the organs being examined, the images are often more precise than those obtained with abdominal scanning alone and small details can be easier to track.
In infertility, this investigation is frequently included from the start because one examination can answer multiple practical questions: what the uterine cavity looks like, what the endometrium looks like at that time, how the ovaries appear and whether there are findings that may influence the plan, such as cysts, polyps, fibroids or signs compatible with endometriosis.
What a Transvaginal Ultrasound Can Show Before IVF: Key Findings That May Influence Planning
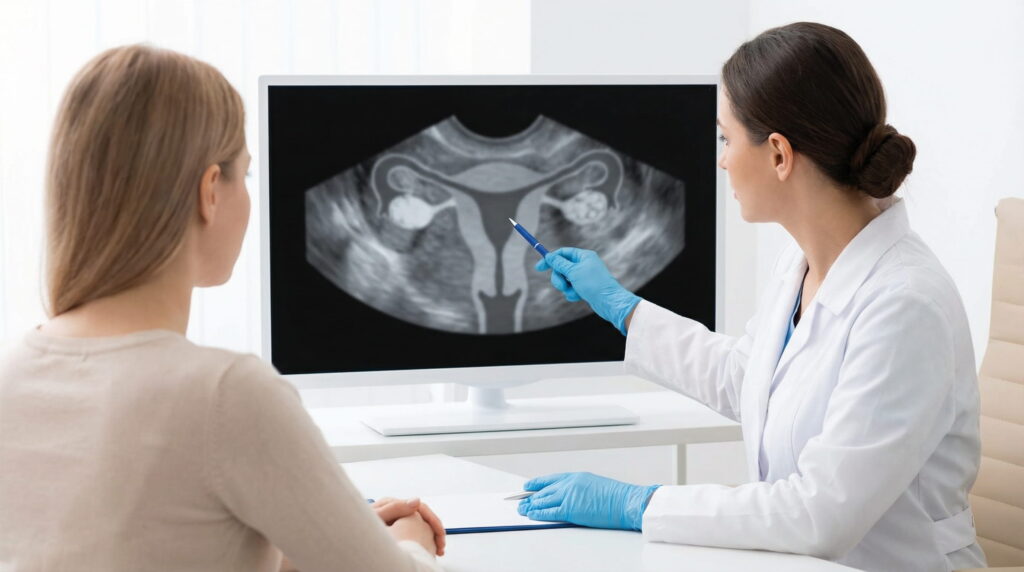
Before IVF, a transvaginal ultrasound is generally used to understand the starting “baseline.” Some findings are mainly orienting, while others indicate the need for confirmation through dedicated investigations. The essential point is interpretation in context, without rushed conclusions.
Ovaries and the “Visible” Ovarian Reserve
A common ultrasound reference is the antral follicle count (AFC), used as an orienting indicator of ovarian reserve. Practically, the scan can show how many small follicles are visible in each ovary and this information is correlated with hormonal tests and age.
In initial evaluation, ultrasound is often complemented by standard blood tests that help outline the biological picture. For a broader overview of baseline investigations, the female fertility test page may be relevant.
Ovarian Cysts and Signs Suggestive of Endometriosis
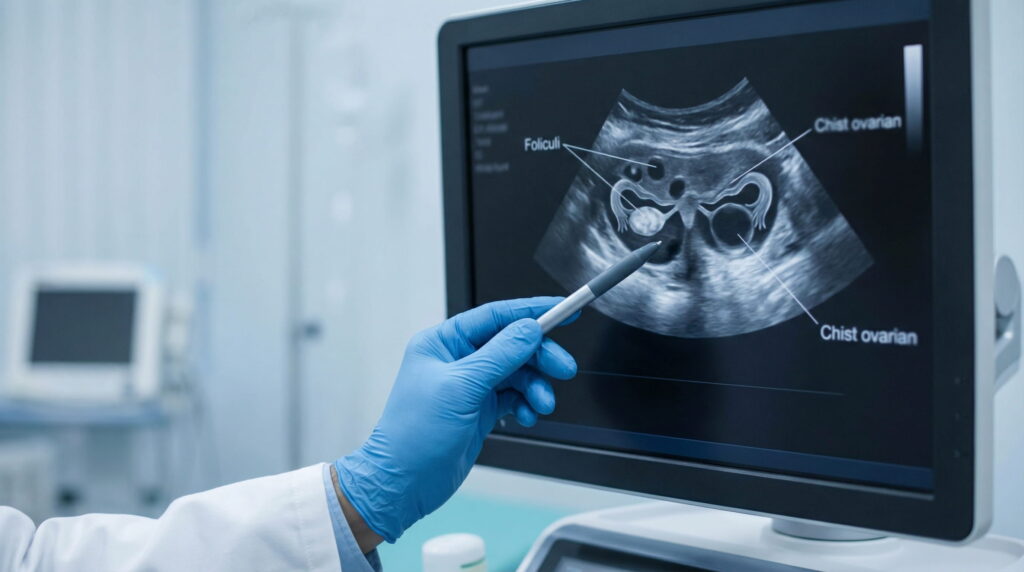
A transvaginal ultrasound may identify functional cysts, which can appear normally at certain times in the cycle, but also findings that require more careful interpretation. Sometimes signs compatible with endometriosis can be present, such as a cyst with an appearance suggestive of an endometrioma, and in this context ultrasound becomes an important piece of the clinical puzzle.
Because symptoms can significantly guide interpretation, such as pelvic pain, painful periods, pain during intercourse or cyclic digestive symptoms, structured information about endometriosis symptoms may also be useful.
The Uterus and the Uterine Cavity
Before IVF, uterine assessment focuses on both the general aspect (size, contour, position) and possible changes affecting the uterine cavity. The scan can look for fibroids, especially if they may distort the cavity, suspicion of endometrial polyps or other anatomical particularities.
These findings do not automatically represent an obstacle, but they may determine whether a further evaluation such as sonohysterography or hysteroscopy is useful before starting the protocol, in order to optimize conditions.
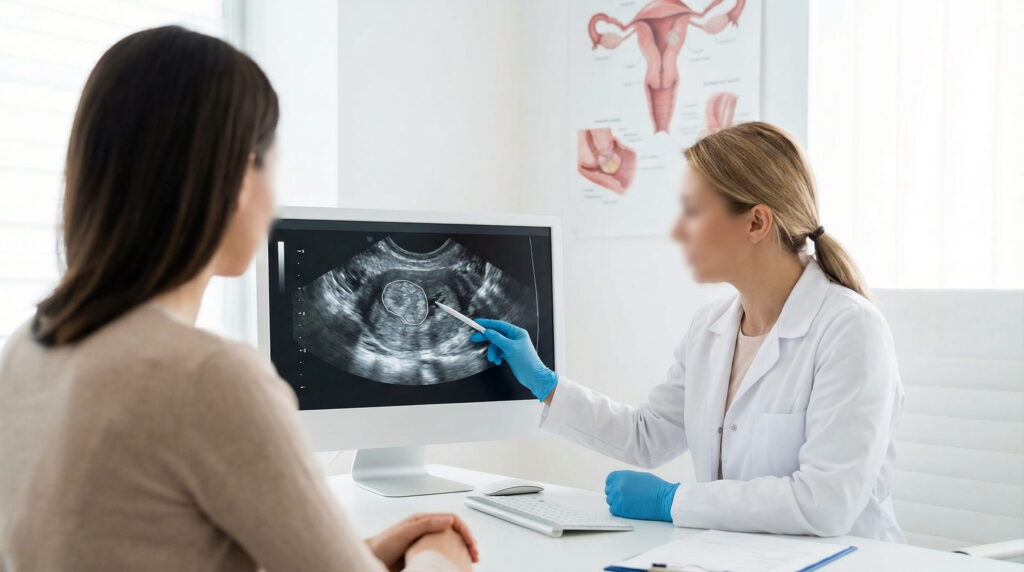
The Endometrium: Thickness and Appearance by Cycle Day
The endometrium can only be interpreted correctly in the context of the menstrual cycle day. In some phases it is normal to be thin, in others it thickens and has a characteristic appearance. Before IVF, the scan checks whether endometrial appearance matches the cycle timing and whether there are signs suggesting focal changes.
Often, the same value, such as thickness, can be “normal” on one day and “unusual” on another. For this reason, repeating the exam at a different time or monitoring dynamically may be recommended.
The Cervix and Other Details With Practical Relevance
In certain situations, a transvaginal ultrasound can provide clues about uterine position, such as anteverted or retroverted, and about anatomical details that can matter practically for intrauterine procedures. These are not “problems” in themselves, but information that can help the medical team plan steps more efficiently and comfortably.
When Transvaginal Ultrasound Is Done Before IVF
The optimal timing depends on the objective of the investigation.
For a baseline evaluation, early cycle after menstruation is often preferred, when the endometrium is thin and the ovaries can be assessed more clearly. For monitoring, during stimulation or follicle tracking, ultrasounds are scheduled according to the protocol and individual response.
“You deserve to be heard, seen, treated with respect, and supported throughout your life.”


Preparation and What the Examination Is Like
In most cases, preparation for a transvaginal ultrasound is simple. Special measures are usually not required, but there may be specific recommendations depending on the reason for the exam and medical history.
When it is useful as a practical list, a few key points:
- the bladder is usually empty unless otherwise indicated
- if there is pelvic pain, unusual bleeding or ongoing treatments, this information is useful before the exam
- when monitoring within a protocol, scheduling follows the calendar set by the physician
The procedure itself usually takes a few minutes. The probe is covered, gel is used and the examination is performed with attention to comfort. If discomfort occurs, it should be communicated, because the technique can be adjusted.
How to Read the Report: What Common Conclusions Mean (and What They Do Not Mean)
A transvaginal ultrasound report includes descriptive terms that can seem technical. In reality, many formulations only make sense together with medical history, cycle day and the objective of the scan, whether baseline, monitoring or clarification.
Several ideas support correct interpretation:
- “normal” has different meanings depending on the cycle moment
- one ultrasound captures a “snapshot,” and sometimes comparison over time is needed
- some findings are common and benign, such as functional cysts, while others require clarification
Before IVF, these details are usually correlated with blood tests and the rest of the evaluation to avoid decisions based on a single element.
The Patient Experience: Why Comfort and Clear Explanations Matter
Even if the exam is short, the way it is explained and how conclusions are discussed can strongly influence the experience. In fertility evaluation, anxiety is common and clear explanations reduce misinterpretation and unnecessary stress.
For a perspective focused on the real-life journey and the human side of treatment, the IVF patient experience page may be relevant.
Frequently Asked Questions
Is transvaginal ultrasound painful?
Most of the time, a transvaginal ultrasound is perceived as uncomfortable rather than painful. Discomfort can vary depending on sensitivity, inflammation or muscle tension. If pain occurs, the examination can be adapted.
Can transvaginal ultrasound be done during menstruation?
It depends on the objective. For certain evaluations, early cycle can be useful. If bleeding is heavy or the goal is different, rescheduling may be recommended.
Do you need a full bladder for transvaginal ultrasound?
Usually, no. In many situations an empty bladder is preferred for comfort and visualization. If there is a special indication, it will be communicated beforehand.
How long does a transvaginal ultrasound take?
In most cases, a few minutes up to about 10 to 15 minutes, depending on complexity and what needs to be assessed.
What can a transvaginal ultrasound say about ovarian reserve?
It can estimate the antral follicle count (AFC), an orienting marker of ovarian reserve. This information is interpreted together with hormonal tests and the clinical context, not as an isolated verdict.
If a polyp or fibroid is seen, can IVF still be started?
In many situations, yes, but it depends on location, size and impact on the uterine cavity. Sometimes additional investigations or treatment are recommended before starting the protocol to optimize conditions.
Can transvaginal ultrasound suggest endometriosis?
Sometimes signs can be suggestive, but diagnosis is based on the full clinical picture and, when needed, further investigations. For a general overview, the endometriosis page about what it is, causes, symptoms and treatment may be useful.
How often is transvaginal ultrasound done during IVF monitoring?
Frequency depends on the protocol and individual response. Monitoring is generally done at intervals set by the physician to assess follicle and endometrial development and adjust treatment when necessary.

The Role of Dr. Andreas Vythoulkas in Transvaginal Ultrasound Before IVF
In clinical practice, a transvaginal ultrasound is not an end in itself. It is one piece of a broader picture: history, symptoms, blood tests and treatment goals. Dr. Andreas Vythoulkas’ role is to integrate this information into a coherent plan, with clear explanations and well-grounded decisions tailored to the specific case.
When ultrasound raises additional questions, such as suspected endometriosis, uterine cavity changes or persistent cysts, the next steps are chosen rationally. Sometimes monitoring is sufficient, other times dedicated investigations are indicated. And when the context is infertility and the goal is a pathway toward IVF, the objective remains the same: safety, clarity and real chances supported by complete evaluation.
For an institutional perspective on treatment, the Genesis Athens page about IVF may also be consulted, and for imaging service context, the transvaginal ultrasound page can complement general information.
Talk to me about
Transvaginal Ultrasound Before IVF

Sources
Similar Articles

Ovarian Retrieval: How the Procedure Works, Pre- and Post-Procedure Recommendations

AMH and Ovarian Reserve: How I Interpret the Values and What They Mean
