When you search for “endometriosis symptoms,” you are most likely doing so not out of simple curiosity, but because the pain has become hard to bear, because it drains you month after month, or because you feel that something isn’t right, yet you still don’t have a clear answer. For many patients, these endometriosis symptoms mean more than menstrual pain. Endometriosis is a common condition, but unfortunately it is often underdiagnosed, precisely because endometriosis symptoms can vary greatly from one woman to another.
In this article you will find, explained in a way that is easy to understand, what the most common endometriosis symptoms are, which warning signs should prompt you to see a doctor, how the diagnosis is established, and what treatment options exist today. If you already have a diagnosis or a strong suspicion, I also recommend reading the page dedicated to endometriosis treatment, where I explain the possible approaches depending on your goal—pain control, protecting fertility, or improving quality of life.
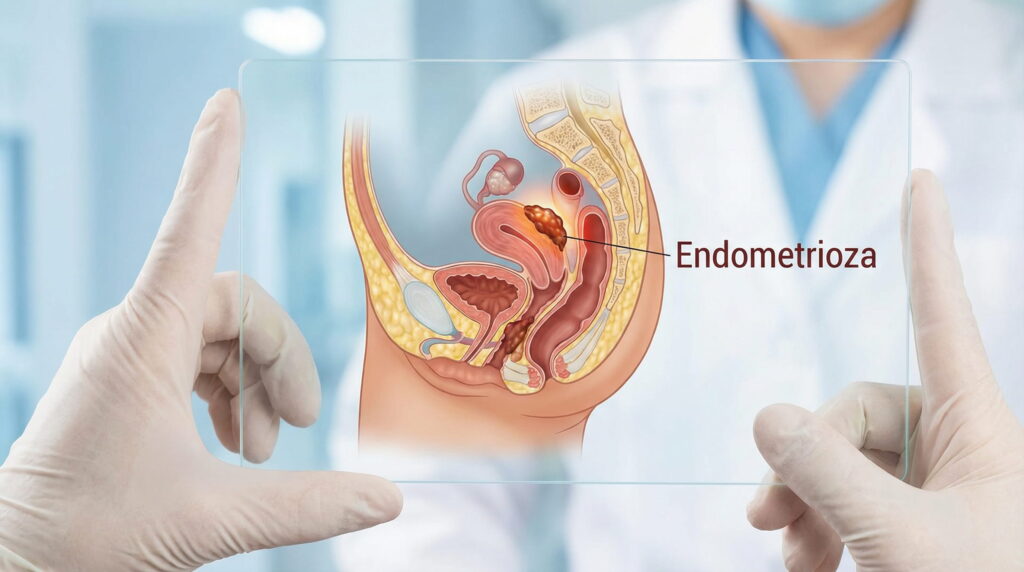
What is endometriosis?
Endometriosis is a condition in which tissue similar to the endometrium (the lining that covers the inside of the uterus) develops outside the uterus. These “islands” of tissue can appear on the ovaries, fallopian tubes, the peritoneum and, sometimes, in deeper areas of the pelvis. Each month, this tissue reacts to hormonal changes, which can cause inflammation, pain and, over time, the formation of adhesions.
It is important to know that endometriosis does not mean only “period pain.” For many patients, the range of endometriosis symptoms also includes digestive, urinary manifestations, or pain during sexual intercourse. Each woman may experience the disease differently, and the intensity of pain does not always reflect the severity of the condition.
Why is endometriosis sometimes diagnosed late?
A common reason is the tendency to normalize pain: “that’s how menstruation is, it has to hurt.” In reality, pain that takes you out of your routine month after month is not normal and should not be ignored. In addition, in the case of endometriosis symptoms, these can vary, and sometimes they are mistaken for other digestive or urinary conditions.
The good news is that, when symptoms are correctly recognized and carefully evaluated, it is possible to reach a correct diagnosis sooner and an effective treatment plan. The earlier we intervene, the higher the chances of controlling the disease and improving quality of life.
Endometriosis symptoms: the most common manifestations (and when they become a warning sign)
When we talk about endometriosis symptoms, we refer to a set of signs that usually recur cyclically, around menstruation, but that can also appear at other times of the month.

- Severe menstrual pain (dysmenorrhea) that affects your life
If the pain keeps you in bed, affects your professional activity, your sleep, or forces you to constantly take anti-inflammatories, this is one of the most important endometriosis symptoms that deserves medical evaluation. Intense pain is not a “normal price” of femininity. - Chronic pelvic pain or pain that returns cyclically
Many patients describe constant pressure in the pelvic area, a dull pain or cramps that begin before menstruation and persist after it ends. These pains can be exhausting and can significantly affect overall well-being. - Pain during sexual intercourse (dyspareunia), especially deep pain
It is a common symptom, but often kept silent. If the pain appears repeatedly, it should not be ignored and should not be “endured.” It is a signal that your body is telling you something is not right. - Digestive symptoms that worsen during menstruation
Severe bloating (“endo belly”), constipation, diarrhea, pain during bowel movements or abdominal discomfort can be part of the picture of endometriosis symptoms, especially when lesions affect intestinal areas. These manifestations can be confused with irritable bowel syndrome, which is why a careful evaluation is important. - Cyclical urinary symptoms
Discomfort when urinating, a sensation of bladder pressure or the frequent need to urinate, especially around menstruation, can be signs of a form of endometriosis that involves the urinary bladder. - Heavy bleeding and pronounced fatigue
Heavy periods, bleeding between periods and persistent fatigue can be associated with other endometriosis symptoms, especially when the pain is severe and repetitive. These can also lead to anemia, which worsens the state of exhaustion.
When to see a doctor (clear signs)
It is time to request a medical evaluation if:
- pain prevents you from carrying out your usual activities;
- you have pain during intercourse or persistent pelvic pain;
- you notice digestive or urinary symptoms that worsen cyclically;
- you have been trying to achieve a pregnancy for 6–12 months (depending on age) without success.

“You deserve to be heard, seen, treated with respect, and supported throughout your life.”


Endometriosis and fertility: how it relates to symptoms and chances of pregnancy
Not all women with endometriosis have fertility problems. However, endometriosis can reduce the chances of pregnancy through inflammation, anatomical changes (adhesions), tubal damage, or the formation of ovarian endometriomas. Sometimes, the first endometriosis symptoms noticed are pain and fatigue; other times, the problem becomes evident only when pregnancy is delayed.
If you want to understand what the journey looks like for a couple who reaches assisted reproduction, I invite you to read in vitro fertilization (IVF) – the patient experience, where I explain step by step the process, the emotions involved, and realistic expectations.
For a more extensive, guide-style overview, you can also consult IVF – complete guide.
The endometrium: why it comes up so often in discussions about endometriosis symptoms
Although endometriosis means the presence of “endometrium-like” tissue outside the uterus, the conversation often also turns to the endometrium, especially when there are concerns related to implantation, irregular bleeding, or infertility.
For a clear and easy-to-understand explanation, you can read the article Everything about the endometrium.
If you are particularly interested in the role of the endometrium in implantation and chances of pregnancy, I also recommend the guide Everything you need to know about the endometrium.
And if there are suspicions of infertility, it is worth consulting the material about Endometrial conditions that can cause infertility.
Diagnosis: how you arrive at the right answer
When the pattern of endometriosis symptoms is suggestive, diagnosis begins with a careful and structured evaluation:
1) Medical discussion and symptom history
A symptom journal is extremely useful: note when the pain occurs, how long it lasts, what makes it worse, what relieves it, and how digestive or urinary symptoms manifest around menstruation. These details can guide the doctor toward a more accurate diagnosis.
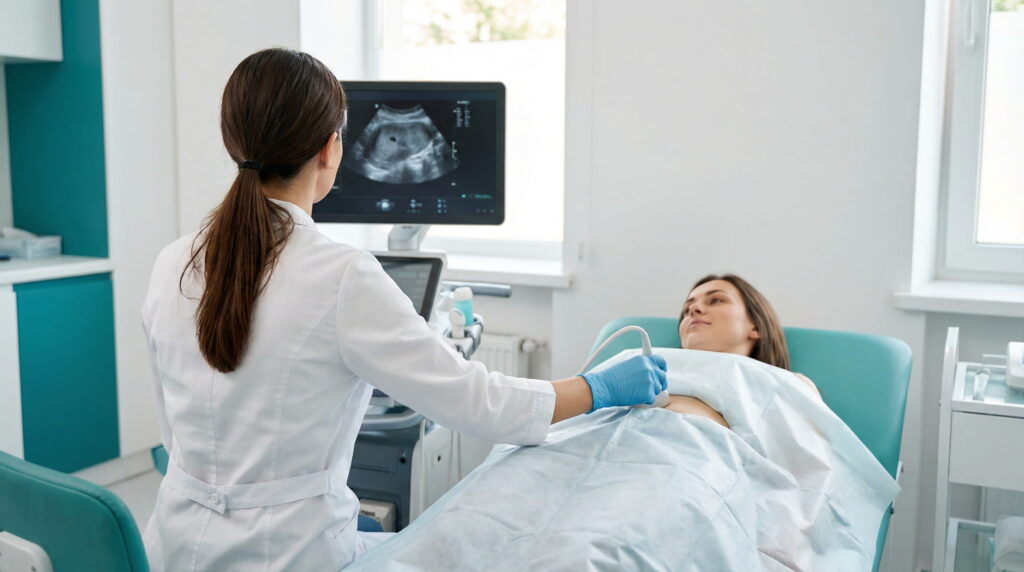
2) Gynecological examination and transvaginal ultrasound
A transvaginal ultrasound performed by an experienced doctor can identify endometriomas and may suggest certain forms of endometriosis. It is a non-invasive investigation, but very valuable.
3) Additional investigations, when needed
In some cases, a pelvic MRI can provide additional information, especially when deep endometriosis is suspected.
4) Laparoscopy (in selected cases)
This can have both a diagnostic and therapeutic role. The decision is made individually, depending on symptoms, age, and the patient’s goals. The aim is to choose the most appropriate approach for you.
Ce puteți face până ajungeți la consult (fără „remedii-minune”)
- Țineți un jurnal al simptomelor (ciclu, intensitatea durerii, medicamente, simptome digestive/urinare, impact asupra somnului și activităților).
- Notați întrebări clare pentru consult: „Care este suspiciunea?”, „Ce investigații sunt potrivite pentru mine?”, „Ce opțiuni am dacă îmi doresc o sarcină?”
- Nu vă învinovățiți dacă vă simțiți epuizată: durerea cronică consumă energie fizică și emoțională, iar acest lucru este un motiv valid pentru a căuta ajutor.
Treatment: what options exist (pain vs. fertility)
The treatment plan depends on symptom intensity, lesion location, age, and reproductive plans.

1) Pain control
Anti-inflammatory medications and pain management strategies can be helpful, especially as temporary support. It is important not to remain stuck in a cycle of “surviving every month” without a clear plan.
2) Hormonal treatment
In many cases, hormonal treatment reduces pain and stabilizes the disease. It is not a definitive “cure,” but it can be an effective solution for controlling endometriosis symptoms, especially when the immediate goal is not achieving a pregnancy.
3) Laparoscopic surgery (when indicated)
It may be recommended in selected situations—severe pain, large endometriomas, suspicion of deep endometriosis, or a significant impact on fertility. The aim is the correct excision of lesions and symptom reduction, while protecting ovarian function.
4) When the goal is pregnancy
If you want to become pregnant, the strategy may include a complete evaluation and, when appropriate, assisted reproduction.
For an institutional perspective on options and the clinical pathway, I also recommend consulting the endometriosis treatment page.
If you want a complete presentation in a guide format, you can also read Endometriosis – what it is, causes, symptoms, and treatment.
What you can do until your appointment (without “miracle remedies”)
- Keep a symptom journal (cycle, pain intensity, medications, digestive/urinary symptoms, impact on sleep and daily activities).
- Write down clear questions for the consultation: “What is the suspicion?”, “Which investigations are appropriate for me?”, “What options do I have if I want a pregnancy?”
- Do not blame yourself if you feel exhausted: chronic pain consumes physical and emotional energy, and this is a valid reason to seek help.
Frequently Asked Questions
What are the most common endometriosis symptoms?
Severe menstrual pain, recurrent pelvic pain, pain during sexual intercourse, cyclical digestive or urinary symptoms, and pronounced fatigue.
Can I have endometriosis if the ultrasound is normal?
Yes. Some forms are not easily seen on ultrasound. Diagnosis is based on symptoms, clinical examination, the doctor’s experience, and additional investigations.
Does endometriosis automatically mean infertility?
No. Many women become pregnant without difficulty, but endometriosis can reduce the chances in certain situations. Individual evaluation is essential.
Does hormonal treatment cure endometriosis?
It can control symptoms effectively, but in some patients symptoms may return after stopping treatment. The plan is adapted to each person’s goals.
When is surgery recommended?
When pain is severe and does not respond to conservative treatments, when there are endometriomas or suspicion of deep endometriosis, or when fertility is affected.
Can endometriosis come back after treatment?
Yes, in some cases endometriosis can recur, especially if hormonal treatment is stopped or if contributing factors persist. Periodic monitoring is important.
Are there lifestyle changes that can help?
Yes, a balanced diet, moderate physical exercise, and stress management can help reduce inflammation and improve symptoms.
Can endometriosis be prevented?
There is no sure method of prevention, but early diagnosis and appropriate treatments can limit disease progression and reduce symptom severity.

The Role of Dr. Andreas Vythoulkas in Managing Endometriosis Symptoms
În contextul endometriozei, rolul meu, ca medic ginecolog specializat în infertilitate, nu se limitează la stabilirea unui diagnostic sau la prescrierea unui tratament standard. Endometrioza este o afecțiune complexă, care necesită o abordare personalizată, comunicare constantă și decizii medicale adaptate fiecărei paciente, în funcție de simptome, vârstă și obiectivele de viață.
În cadrul consultațiilor, scopul meu este să clarific diagnosticul real, să explic opțiunile de tratament disponibile și să ajut fiecare femeie să înțeleagă care este cea mai potrivită strategie pentru ea – fie că vorbim despre controlul durerii, despre protejarea fertilității sau despre obținerea unei sarcini. Discutăm deschis despre alternative, despre șansele reale de succes, despre limitele biologice și despre ce presupune concret fiecare etapă a tratamentului, nu doar din punct de vedere medical, ci și emoțional.
Pe parcursul tratamentului, este esențial ca pacienta să nu se simtă singură într-un proces care poate fi solicitant. De la stabilirea diagnosticului și monitorizarea evoluției, până la intervențiile chirurgicale sau planurile de fertilitate, rolul meu este să ofer explicații clare, să ajustez strategia atunci când este necesar și să asigur continuitatea îngrijirii.
Poate cel mai important aspect al acestui parcurs este încrederea și colaborarea. Endometrioza nu se rezolvă întotdeauna într-o singură etapă, iar uneori este nevoie de reevaluare și răbdare. În aceste momente, relația medic–pacient devine esențială: discutăm deschis despre evoluția bolii, despre impactul asupra calității vieții și despre opțiunile reale care există mai departe.
Obiectivul meu nu este doar ameliorarea simptomelor, ci construirea unui plan coerent, realist și sigur, care să redea pacientelor controlul asupra propriei vieți. Endometrioza nu este doar o afecțiune medicală, ci o experiență de viață, iar rolul medicului este să fie un partener de încredere pe tot parcursul acestui drum.
Talk to me about
Endometriosis Symptoms

Sources
Similar Articles

Reproductive Planning: What I Tell Patients Who Want to Delay Pregnancy

Embryo Donation | Medical Perspectives
