An endometrial polyp is one of the changes I frequently encounter when evaluating patients who are dealing with abnormal uterine bleeding, difficulty conceiving or investigations carried out before In Vitro Fertilization (IVF). In many cases, this lesion is first observed on transvaginal ultrasound, but its relevance is not the same in every case.
In my practice, I discuss an endometrial polyp not only as a simple imaging diagnosis, but as a possible cause that may influence endometrial receptivity and embryo implantation. Sometimes, an endometrial polyp is an incidental finding and can simply be monitored. At other times, especially in infertility or before reproductive treatments, this lesion becomes important and must be analyzed carefully.
That is why I think it is useful to explain very clearly what an endometrial polyp is, how it can affect fertility and when I recommend intervention. In reality, the correct decision is not based only on the presence of the lesion, but on its size, location, symptoms, hormonal context and the patient’s reproductive plan.
What an endometrial polyp is and how it appears
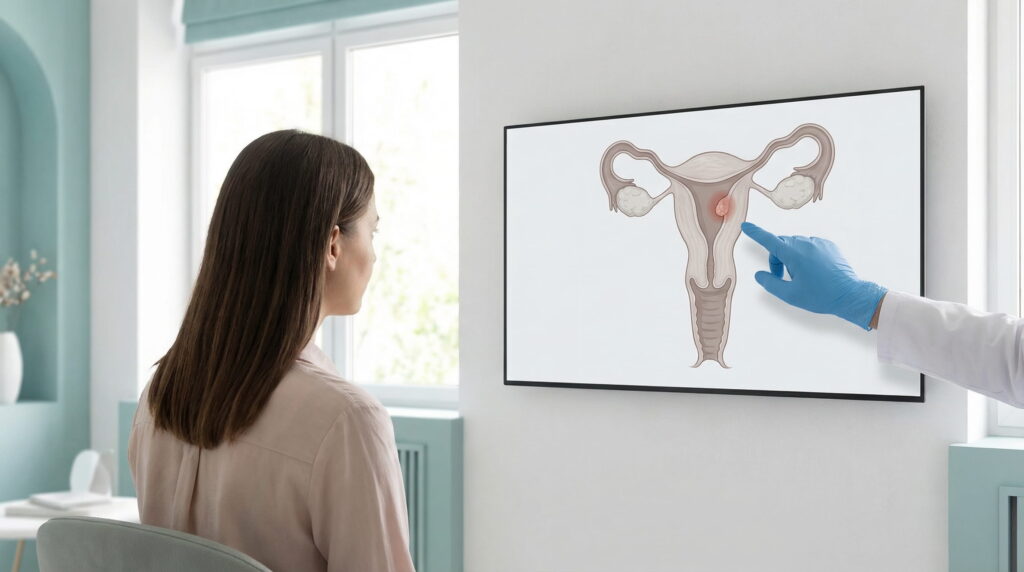
An endometrial polyp is a localized proliferation of the endometrium, meaning the lining that covers the inside of the uterus. This formation develops inside the uterine cavity and can vary greatly in size. Some endometrial polyps remain small and stable, while others grow, cause symptoms or influence the environment in which implantation should take place.
In more general language, the expression uterine polyps is sometimes also used, but the correct and more medically precise term is endometrial polyp, because it describes the exact site from which the lesion originates. Its appearance is linked to the endometrium’s response to hormonal stimuli, especially estrogenic ones, and the frequency of these formations increases with reproductive age.
From a clinical point of view, it is not enough to know that there is an endometrial polyp. What matters a great deal is where it is located and whether it alters the shape of the uterine cavity. In certain cases, for a clearer picture of the cavity, I may recommend Sono-HSG, especially when standard ultrasound raises suspicion but does not provide all the necessary details.
What symptoms endometrial polyps can cause
Not all patients with endometrial polyps have obvious symptoms. Sometimes, an endometrial polyp is discovered by chance during an evaluation performed for infertility or before treatment. In other situations, it is precisely the symptoms that bring the patient to the doctor.
The most common manifestation is abnormal uterine bleeding. This may include spotting between periods, prolonged bleeding, heavier menstruation or small amounts of bleeding before or after menstruation. Sometimes, the patient has no pain and does not associate these changes with an intrauterine problem, but a symptomatic endometrial polyp always deserves careful evaluation.
There are also patients in whom uterine polyps do not cause obvious signs, but are identified in the context of more complex investigations. In infertility, this situation is common, including in treatment journeys involving reproductive procedures, where a correct understanding of every stage, including the patient experience, plays an important role in medical decision-making.
How an endometrial polyp can affect implantation
An endometrial polyp can influence implantation because it locally changes the surface of the endometrium and may disrupt the environment required for embryo attachment. Implantation is a delicate process, dependent on the synchronization between the embryo and endometrial receptivity, and any intracavitary formation may interfere with this balance.
Beyond its simple mechanical presence, an endometrial polyp may also be associated with local vascular changes and with an inflammatory microenvironment that reduces the quality of implantation. I do not claim that every endometrial polyp prevents pregnancy, because that would not be medically correct. What I do say is that there are situations in which an endometrial polyp becomes a real obstacle and must be treated as such.
This aspect is important both in natural conception and in assisted reproduction. When I discuss success chances in an In Vitro Fertilization (IVF) cycle, I consider the correct evaluation of the uterine cavity to be one of the stages that should never be treated superficially.
When an endometrial polyp becomes a fertility problem
Not every endometrial polyp has the same relevance. In practice, I am interested in size, location, persistence over time, symptoms and the patient’s reproductive history. A small, peripheral and asymptomatic endometrial polyp may have limited impact. By contrast, an endometrial polyp located in an area that distorts the uterine cavity or appearing in a patient with infertility must be viewed much more carefully.
The clinical context makes the difference. There are situations in which endometrial polyps coexist with other gynecological problems that influence fertility, and then the evaluation must be integrated. This is especially true when we are discussing conditions such as endometriosis and the role of endometriosis treatment in the patient’s reproductive plan.
In addition, when there have been repeated implantation failures or several unsuccessful attempts, an endometrial polyp should not be ignored just because it appears small. Sometimes, its impact is disproportionate to its size, and that is exactly why it must be judged according to the entire context, not in isolation.
“You deserve to be heard, seen, treated with respect, and supported throughout your life.”


How it is correctly diagnosed
Diagnosis most often begins with ultrasound. Still, standard ultrasound does not always provide all the answers. When the image raises suspicion or when I need a more precise evaluation of the uterine cavity, the next step may be an additional investigation or a direct visualization method.
The method that offers the greatest precision is hysteroscopy. It allows direct visualization of the uterine cavity, confirmation of the diagnosis of endometrial polyp and, in many situations, treatment during the same stage. That is exactly why I consider hysteroscopy one of the most valuable procedures when we want a clear diagnosis and a well-argued management plan.
For patients who want to better understand why this procedure has such an important role in infertility and in the evaluation of intracavitary pathology, the article about hysteroscopy: why it is essential naturally complements this discussion.
When I recommend intervention
I do not recommend treatment automatically just because an endometrial polyp has been identified. In my practice, intervention is justified when the formation has real clinical impact: it causes bleeding, persists, grows, distorts the uterine cavity or appears in a context in which implantation needs to be optimized.
There are several situations in which the recommendation for treatment becomes clearer:
- when an endometrial polyp is symptomatic
- when there is infertility or implantation failure
- when embryo transfer is planned
- when the uterine cavity does not have a favorable appearance
- when the lesion persists on re-evaluation
On the other hand, there are also cases in which monitoring is reasonable. A small endometrial polyp without symptoms in a patient without an immediate reproductive goal may be followed. Still, when pregnancy is being pursued, my threshold for tolerance is lower, because I try to reduce as much as possible the factors that may negatively influence implantation.
What follows after removal of an endometrial polyp
After removal of an endometrial polyp, the strategy depends on the clinical context. Sometimes, a short healing period is enough and pregnancy can then be attempted naturally. At other times, especially in infertility, I reassess the uterus and determine the optimal moment for continuing treatment.
At this stage, it is important for me to make sure that the endometrium has a favorable appearance and that the uterine environment is as well prepared as possible. In a broader therapeutic journey, the information in In Vitro Fertilization (IVF): complete guide connects very well with this stage, because success depends not only on the embryo, but also on the quality of the uterine cavity.
In addition, follow-up may require a new imaging evaluation. For this reason, it is also useful to understand the role of transvaginal ultrasound in patient monitoring, especially in infertility and before resuming therapeutic steps.
Endometrial polyp and other associated causes of infertility
In practice, there is rarely a single clear cause of infertility. An endometrial polyp may be the main factor or it may appear alongside other pathologies. That is exactly why I always try not to oversimplify. Fertility is influenced by egg quality, tubal patency, hormonal status, the uterus and many other elements that must be analyzed together.
In certain situations, endometrial polyps are associated with conditions such as endometriosis, and the evaluation must be done within an integrated logic. From this perspective, the discussion about endometriosis treatment naturally connects with fertility optimization and with preparing a uterus that is as balanced as possible for implantation.
Also, when the patient is preparing for reproductive treatment, repeated ultrasound evaluation plays an important role. In this context, the article about transvaginal ultrasound in infertility, before IVF adds clarity to the understanding of the steps that precede embryo transfer.
Frequently Asked Questions
Does an endometrial polyp always prevent pregnancy?
No. An endometrial polyp does not automatically block pregnancy, but in certain cases it may reduce implantation chances and may justify treatment.
Can endometrial polyps go away on their own?
Some small endometrial polyps may regress, but this should not be assumed without monitoring. If symptoms or infertility are present, evaluation must be done carefully.
When does hysteroscopy become necessary?
Hysteroscopy is indicated when an endometrial polyp needs to be confirmed, precisely evaluated or removed, especially if it influences symptoms or the reproductive plan.
Does a small endometrial polyp always need surgery?
No. A small and asymptomatic endometrial polyp can sometimes be monitored. The decision depends on the clinical context and the reproductive objective.
Do uterine polyps affect IVF?
They can, especially if they alter the intracavitary environment or endometrial receptivity. That is why their evaluation is important before embryo transfer.
How is an endometrial polyp best seen?
Most often, it is suspected on ultrasound and confirmed through hysteroscopy, which allows direct visualization of the uterine cavity.
Can an endometrial polyp return after treatment?
Yes, an endometrial polyp may recur. For this reason, follow-up remains important, especially if symptoms or difficulties conceiving reappear.
Does removing an endometrial polyp increase implantation chances?
In many cases, yes, especially when that endometrial polyp affects the uterine cavity or is considered clinically relevant in the context of infertility.

The role of Dr. Andreas Vythoulkas in evaluating and managing endometrial polyps
When evaluating an endometrial polyp, I consider it essential to distinguish between an incidental finding and a lesion that truly influences fertility. My role is to determine whether that endometrial polyp or those endometrial polyps affect bleeding, the uterine cavity and the real chances of implantation.
My approach is individualized. I do not treat all uterine polyps the same way and I do not recommend intervention according to a rigid criterion. I am interested in reproductive history, investigation results, symptoms and the stage the patient has reached in her medical journey. Sometimes monitoring is enough. At other times, treatment performed at the right moment may represent an important step in optimizing fertility.
In my practice, the goal is not only the removal of an endometrial polyp, but the integration of this decision into a coherent, well-argued medical plan adapted to the reproductive objective. When we talk about implantation and real chances of pregnancy, the correct evaluation of the uterine cavity can make the difference between incomplete management and a well-constructed one.
Talk to me about
Endometrial Polyps

Sources
- American College of Obstetricians and Gynecologists (ACOG) – The Use of Hysteroscopy for the Diagnosis and Treatment of Intrauterine Pathology
- American Society for Reproductive Medicine (ASRM) – Fertility Evaluation of Infertile Women
- NICHD – Infertility and Fertility
- NHS – Hysteroscopy
- MedlinePlus – Endometrial Polyps
Similar Articles

Why Do Fallopian Tubes Become Blocked? Causes, Symptoms, Complications, Solutions

Fertility Preservation for Cancer Patients
